4.5 Disorders of Urinary Tract
This document outlines common disorders affecting the human urinary tract, including infections, kidney stones, and kidney failure, along with their causes, symptoms, and treatments.
Urinary Tract Infection (UTI)
A UTI is an infection in any part of the urinary system. It is significantly more common in women (50 times more) primarily due to the shorter female urethra (1.5 inches vs. 8 inches in men), which allows bacteria from fecal matter to more easily reach the urethra.
-
Types of UTIs (based on location):
- Urethritis: Infection of the urethra.
- Cystitis: Infection involving the bladder.
- Pyelonephritis: Infection of the kidneys.
- The ureters are rarely the site of infection.
-
Causes: UTIs are typically caused by bacteria.
| Bacteria | Associated Diseases |
|---|---|
| E. coli | Urinary Tract Infection (UTI) |
| N. gonorrhoeae | Urethritis, Gonorrhoea |
| T. pallidum | Syphilis |
- Treatment and Prevention:
- Treatment: Curable with antibiotic therapy.
- Prevention: Drinking plenty of water to flush out bacteria and maintaining good personal hygiene.
Kidney Stones (Nephrolithiasis)
Nephrolithiasis is the condition of having hard, crystalline mineral deposits (stones) that form within the kidney or urinary tract. They can range in size from a grain of sand to a golf ball.
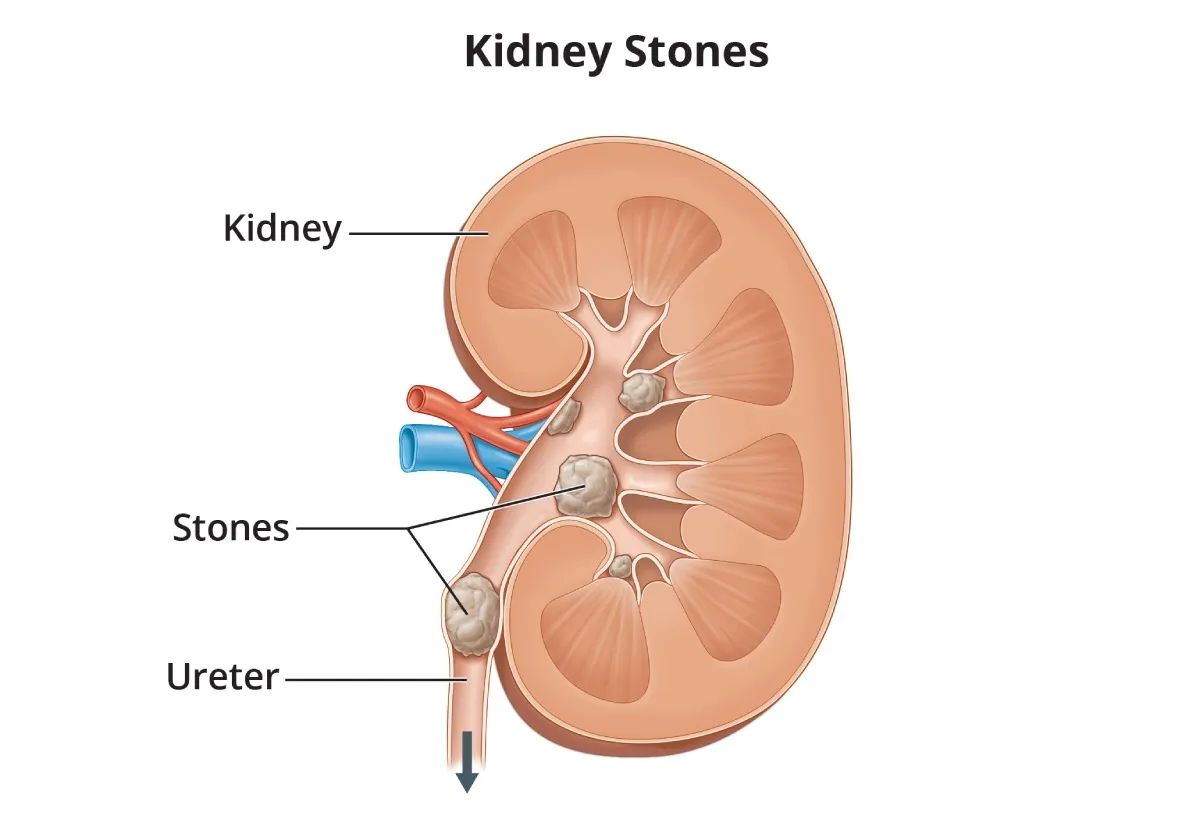
-
Types and Composition:
- Calcium Oxalate: Most common type (70% of patients). Forms when urine is acidic (low pH).
- Calcium Phosphate: Forms when urine is alkaline (high pH).
- Uric Acid: Forms when urine is persistently acidic.
- Magnesium Ammonium Phosphate
- Cystine
- Staghorn stone: A large, branching stone.
-
Symptoms:
- Severe pain in the lower back
- Blood in urine (hematuria)
- Nausea and vomiting
- Fever and chills
- Cloudy or foul-smelling urine
-
Causes:
- Hypercalcemia: Increased calcium level in the blood, leading to hypercalciuria (high calcium in urine).
- Hyperoxaluria: Increased oxalate level in the urine.
- Hyperuricemia: Increased amount of uric acid in the blood.
- High concentration of cysteine and phosphates in urine.
- Continuous dehydration.
-
Treatment:
- Extracorporeal Shock Wave Lithotripsy (ESWL): A non-invasive procedure where an instrument called a lithotripter generates shock waves from outside the body to break the stone into small fragments, which are then passed naturally.
Kidney Failure (Renal Failure)
Kidney failure is a general term for a decline in kidney function, particularly the filtering process. For details on kidney function, refer to Functions of Kidney→.
-
Chronic Renal Failure:
- An irreversible, gradual, and progressive deterioration of renal function over years.
- Causes: Bacterial infections, nephritis (inflammation of glomeruli), damage from high blood pressure, and diabetes mellitus.
- Can progress to end-stage renal disease (ESRD) and uremia (high levels of waste in the blood), which is fatal without treatment.
-
Acute Renal Failure:
- A sudden decline in kidney function.
- Causes: Haemorrhage, severe vomiting/diarrhoea, diuresis (excessive urination), urinary tract obstruction (e.g., kidney stones), severe nephritis.
Treatments for End-Stage Renal Disease (ESRD)
Renal Dialysis
A procedure to artificially filter toxins from the blood when the kidneys can no longer perform this function.
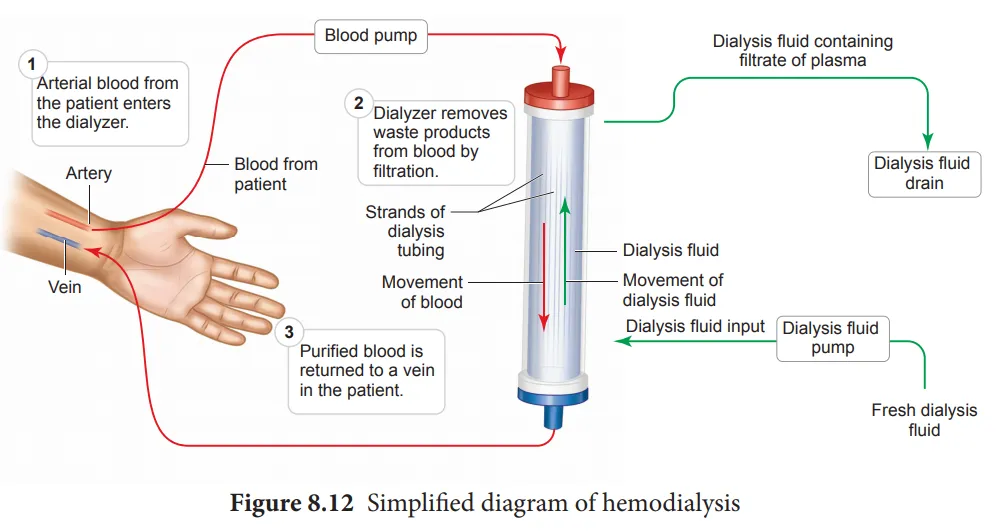
- Haemodialysis:
- Blood is circulated outside the body through an external filter called a dialyzer.
- The dialyzer contains tubes made of a semipermeable membrane (cellophane).
- Blood flows through these tubes while a special fluid called dialysate flows around them in the opposite direction (counter-current flow).
- Wastes, excess salts, and water move from the blood into the dialysate by diffusion, and the cleansed blood is returned to the body.
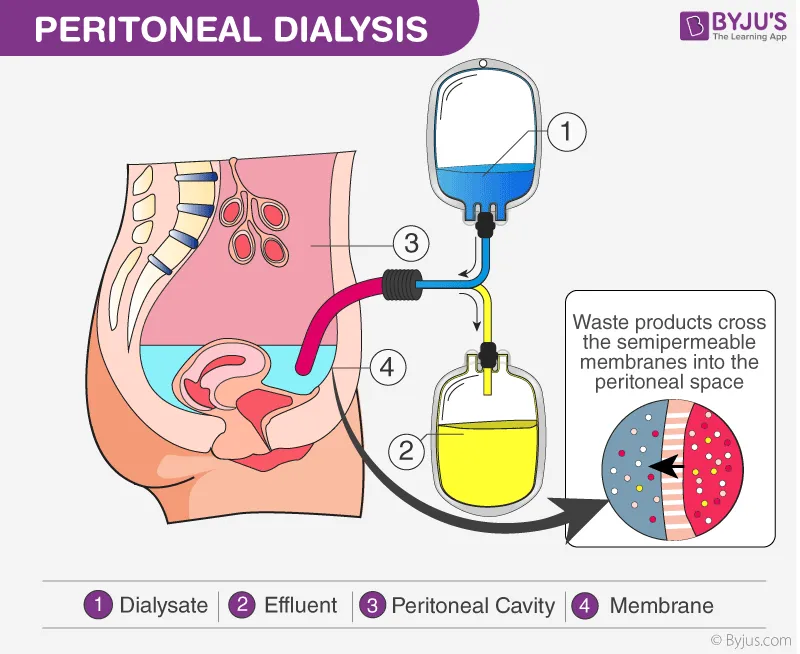
- Peritoneal Dialysis:
- Uses the body's own peritoneum (the membrane lining the abdominal cavity) as a natural filter.
- Dialysate is introduced into the abdominal cavity through a surgically inserted catheter.
- Waste products from the blood in the peritoneal capillaries diffuse into the dialysate.
- The fluid containing the waste is then drained from the abdomen.
Kidney Transplant
A surgical procedure to place a healthy kidney from a donor into a person with chronic kidney failure.
-
Principles of Transplant:
- The donor can be deceased or living (related or unrelated).
- ABO blood group compatibility is essential.
- Matching of Human Leucocyte Antigens (HLA) improves graft survival.
- A person can live a normal life with just one kidney.
-
Problems Associated with Transplant:
- Rejection: The recipient's immune system attacks the new kidney.
- Immunosuppression: Patients must take medications (e.g., cyclosporine) for life to suppress their immune system and prevent rejection. These drugs have toxic side effects.
- Rejection can occur at any time if the medication is stopped.