4.3 Urine Formation
Urine formation is the process by which the kidneys filter blood to remove waste products and excess substances, ultimately producing urine. This involves three primary steps: glomerular filtration, tubular reabsorption, and tubular secretion, primarily occurring within the nephron.
Glomerular Filtration (Pressure Filtration)
- Definition: The first step in urine formation, where blood pressure forces water and small solutes from the blood in the glomerular capillaries into the Bowman's capsule.
- Location: Renal Capsule (Glomerulus + Bowman's Capsule).
- Mechanism:
- Driven by high hydrostatic pressure in the glomerular capillaries.
- This high pressure is generated because the efferent arteriole (leading out) is about half the diameter of the afferent arteriole (leading in), creating resistance to blood flow.
- Filtrate Composition:
- Filtered Substances: Water, ions, glucose, amino acids. The resulting fluid is called glomerular filtrate.
- Substances Retained in Blood: Larger molecules like proteins, red blood cells, and platelets.
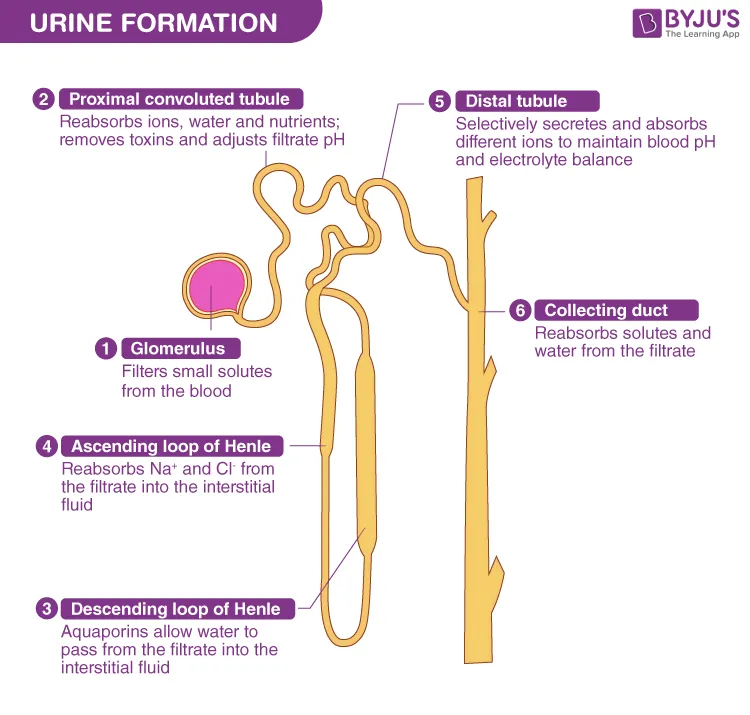
Tubular Reabsorption (Selective Reabsorption)
- Definition: The process where essential substances and water are moved from the filtrate back into the blood via the peritubular capillaries.
- Mechanism: It is a selective process, meaning only needed substances are reabsorbed.
- Reabsorbed Substances: Glucose, amino acids, vitamins, inorganic salts, and a significant amount of water.
Tubular Secretion
- Definition: The process of actively transporting waste products and excess ions from the blood into the filtrate.
- Location: Primarily in the loop of Henle, but also occurs in the convoluted tubules.
- Secreted Substances: Ammonium ions (), hydrogen ions ().
- Purpose: To eliminate additional wastes and, critically, to maintain the pH of the urine and blood. Normal urine pH ranges from 4.8 to 7.5.
Mechanism of Urine Concentration
The ability to produce concentrated (hypertonic) urine is crucial for water conservation.
Countercurrent Multiplier Mechanism:
- Goal: To reabsorb a large amount of water (approximately 99.5%) from the filtrate, concentrating the urine.
- Location: Loop of Henle and Collecting Duct.
- Process:
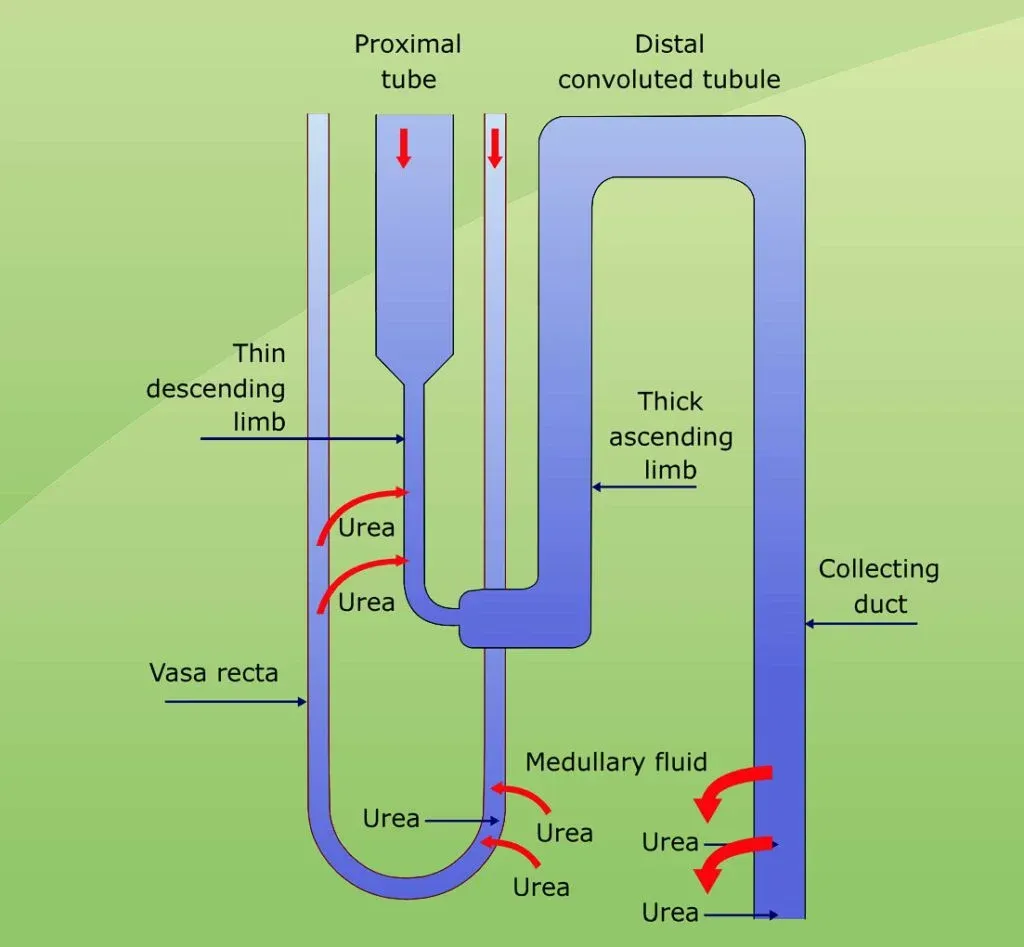
- Countercurrent Flow: Filtrate flows down the descending limb and up the ascending limb of the loop of Henle, while blood in the vasa recta (surrounding capillaries) flows in the opposite direction.
- Ascending Limb: Actively pumps sodium chloride () out into the surrounding kidney tissue (interstitium). This process is regulated by the hormone aldosterone. This makes the interstitium highly concentrated (salty).
- Descending Limb: Is permeable to water but not to salt. As the filtrate moves down, water exits via osmosis into the salty interstitium. This water reabsorption is promoted by Antidiuretic Hormone (ADH).
Types of Nephrons and Capillaries
| Feature | Cortical Nephrons | Juxtamedullary Nephrons |
|---|---|---|
| Abundance | 70-80% of nephrons | 20-30% of nephrons |
| Location | Renal corpuscle in the superficial cortex | Renal corpuscle near the cortex-medulla junction |
| Loop of Henle | Relatively short | Long, extends deep into the medulla |
| Primary Function | Control of blood volume by forming diluted urine under normal water conditions. | Increased water retention by forming concentrated urine when water is in short supply. |
| Feature | Glomerular Capillaries | Peritubular Capillaries |
|---|---|---|
| Primary Function | Filtration of blood plasma to form filtrate. | Reabsorption of essential substances and secretion of waste products. |
| Mechanism | Operates under high pressure to force fluid and solutes out. | Operates under low pressure to allow for reabsorption of nutrients, minerals, and water. |
| Substances Handled | Retains blood cells and large proteins in the blood. | Reabsorb useful minerals and nutrients; secrete waste into the filtrate. |
Other Kidney Functions
Beyond excretion and osmoregulation, kidneys also have endocrine functions:
- Erythropoietin (EPO): A hormone secreted by the kidneys that stimulates the formation of red blood cells.
- Renin: An enzyme secreted by the kidneys that helps regulate blood pressure.
Possible Questions/Answers
-
Q: What are the three main processes of urine formation? A: Glomerular filtration, tubular reabsorption, and tubular secretion.
-
Q: Why does filtration occur in the glomerulus? A: Due to high hydrostatic (blood) pressure, caused by the efferent arteriole being narrower than the afferent arteriole, which forces water and small solutes out of the blood.
-
Q: What is the role of the countercurrent multiplier mechanism? A: It creates a salt concentration gradient in the kidney medulla, which allows for the maximum reabsorption of water from the filtrate, thereby concentrating the urine.
-
Q: How do ADH and Aldosterone affect urine concentration? A: ADH (Antidiuretic Hormone) increases water reabsorption from the descending limb and collecting duct. Aldosterone increases the pumping of salt (NaCl) out of the ascending limb, which enhances the concentration gradient for water reabsorption.